Introduction
Aerobic exercise has emerged as a well-established intervention for enhancing pulmonary function across diverse clinical populations [1,2]. Following cervical and upper thoracic spinal cord injuries (SCI), individuals often experience a spectrum of pulmonary dysfunctions attributed to impaired respiratory muscle performance, including the diaphragm, intercostal muscles, accessory respiratory muscles, and abdominal muscles [3]. Respiratory complications such as reduced lung function and weakness in respiratory muscles are common sequelae of SCI, sometimes necessitating interventions like tracheostomy [4]. However, such interventions can significantly impact long-term respiratory function and diminish the quality of life for affected individuals [4]. In this report, we present a case study detailing the implementation of moderate to high-intensity aerobic exercise as a treatment modality in a spinal cord-injured patient with tracheostomy, aimed at achieving decannulation.
Case Report
A 19-year-old patient was admitted to the hospital following a traffic accident resulting in a spinal cord injury. Imaging studies revealed compression fractures at T4-6, anterior dislocation with facet perching at the right T4/5 facet joint, and a flexion-distraction injury at T4-6. The patient also sustained fractures of the upper sternum, right 4th to 7th ribs, and left 1st rib. Posterior arthrodesis from T3-T7 with decompression was performed. The patient's American Spinal Injury Association Impairment Scale classification was B, with the neurological level of injury at the T4 level. One week after admission, the patient developed left lung collapse, necessitating tracheostomy due to respiratory distress. The patient had no significant medical history. Clinical symptoms included respiratory muscle weakness and lower limb paralysis.
A comprehensive assessment was conducted, evaluating the patient's sensorium, airway patency, swallowing function, need for suction, and spontaneous breathing. During the laryngeal examination, including assessment of vocal cord movement, no abnormalities were detected. The airway was observed to be clear and unobstructed, swallowing functioned effectively, and the patient exhibited intact sensorium. The patient was able to tolerate corking training for more than 24 hours. However, the patient's cough flow was ineffective for decannulation. Initial respiratory function tests revealed compromised lung function: peak cough flow (PCF) was 60 L/min, forced expiratory volume in one second (FEV1) was 1.48 L (50% of predicted), forced vital capacity (FVC) was 2.15 L (56% of predicted), and peak expiratory flow (PEF) was 2.43 L/sec (17% of predicted). Peak cough flow was measured by instructing the patient to take as deep a breath as possible and then cough. With the tracheostomy cuff deflated, a Shiley speaking valve was attached to the tracheostomy tube. The patient used a mouthpiece connected to the peak cough flow meter, and nose clips were applied to ensure accurate measurement.
To facilitate decannulation, the patient underwent a pulmonary rehabilitation intervention, which included diaphragmatic breathing exercises, air stacking maneuvers, and threshold inspiratory and expiratory muscle strengthening exercises. Despite undergoing two months of rehabilitation intervention, respiratory parameters remained suboptimal: PCF was 80 L/min, FEV1 was 1.62 L (55% of predicted), FVC was 2.35 L (62% of predicted), and PEF was 3.27 L/sec (22% of predicted).
During the initial two months after the injury, no significant improvement in pulmonary function was observed. The patient’s general medical condition deteriorated due to a Coronavirus Disease 2019 (COVID-19) infection and Clostridium difficile infection, which required isolation and limited rehabilitation to bedside respiratory training for approximately three weeks. Additionally, a pressure ulcer in the coccygeal area and orthostatic hypotension further prevented the patient from maintaining a sitting position. After stabilization of these conditions, aerobic exercise was incorporated into the rehabilitation program along with conventional respiratory therapy once sitting activities became possible.
Once the patient regained the ability to sit independently in a wheelchair, aerobic exercise using an upper body ergometer was initiated. Guided by the Karvonen heart rate reserve method, the initial target heart rate was set at 130 bpm (40% of heart rate reserve) based on a resting heart rate of 80 bpm. As the patient's cardiopulmonary function improved, the target heart rate was progressively increased to 140 bpm, eventually reaching 153 bpm (60% of heart rate reserve). Each exercise session lasted for 30 minutes and was performed twice daily.
Two weeks after initiating aerobic exercise, PCF increased to 150 L/min, with subsequent measurements after one month showing further improvement: PCF reached 190 L/min. Following this improvement, decannulation was successfully performed. No complications were encountered during aerobic exercise, and post-decannulation respiratory distress was absent. Post-discharge outpatient follow-up assessments indicated sustained respiratory function: peak cough flow was 190 L/min, FEV1 was 2.95 L (100% of predicted), FVC was 3.04 L (80% of predicted), and PEF was 5.61 L/sec (38% of predicted) (Fig. 1 and Fig. 2).
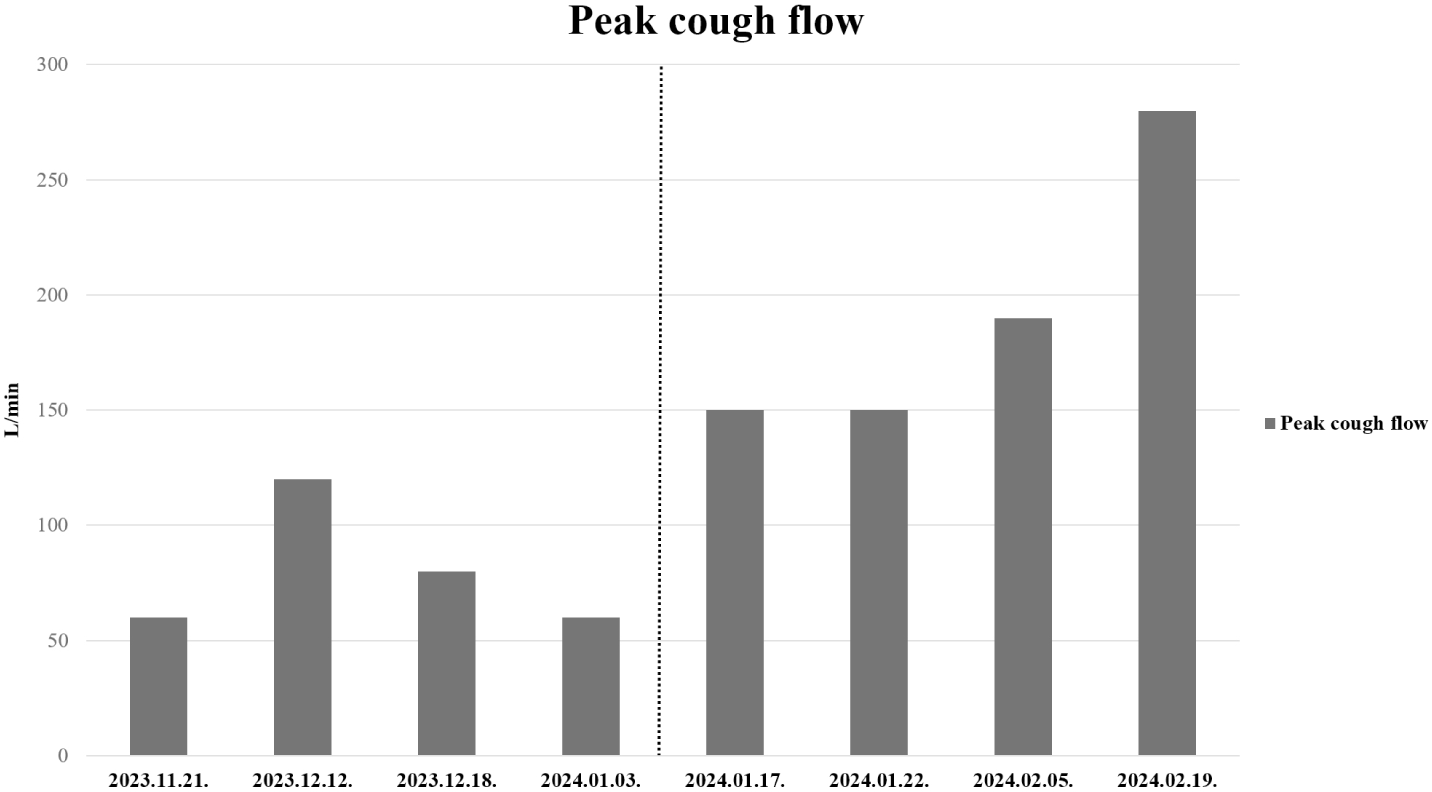
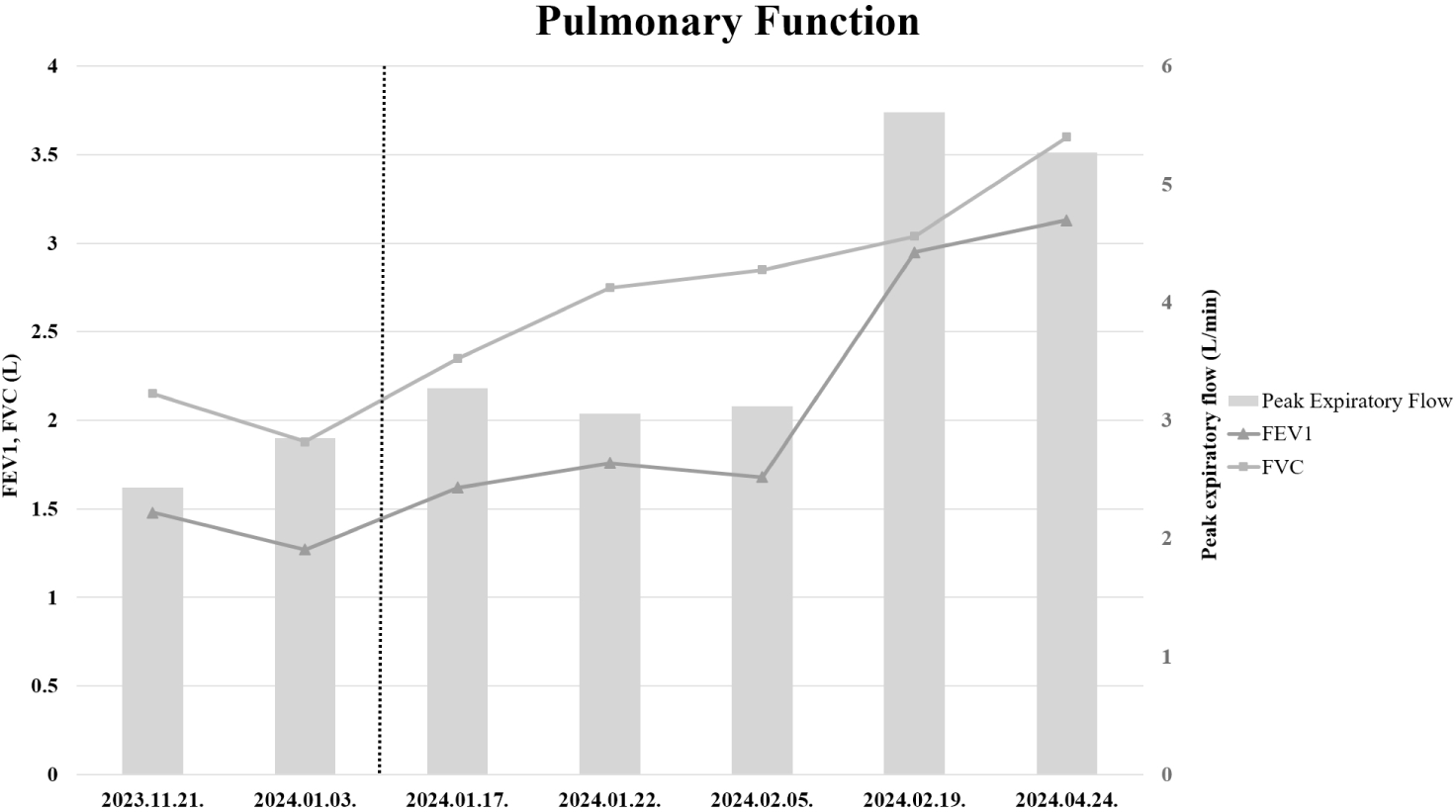
Discussion
In patients with SCI who undergo aerobic exercise, there is a reported positive impact on their quality of life and mental health [5]. However, previous studies have not specifically investigated pulmonary function or PCF. While many studies have explored pulmonary rehabilitation interventions, such as diaphragmatic breathing exercises, air stacking maneuvers, and inspiratory and expiratory muscle strengthening exercises, leading to decannulation [4,6,7], in our case report, conventional rehabilitation therapy alone did not sufficiently improve cough flow for decannulation.
While there is existing research on respiratory muscle training in athletes with cervical spinal cord injury, focusing on cardiopulmonary function and exercise capacity [8], these studies did not evaluate aerobic exercise. Additionally, while previous studies focused on athletes, the patient in this case report was a typical student. Previous studies have demonstrated improvements in pulmonary function and inhibition of alveolar cell apoptosis through aerobic exercise in animal models [9]. In our case report, the improvement in FVC through aerobic exercise suggests an increase in PCF. The enhancement in respiratory performance is likely attributable to strengthening of key respiratory muscles, including the diaphragm, internal and external intercostal muscles, which play a primary role in inspiration and expiration. Aerobic exercise increases the strength and endurance of these muscles, leading to more effective ventilation and improved lung volumes such as FVC and FEV1 [10]. Enhancement of inspiratory muscle strength led to increased lung capacity and improved ventilation-perfusion (V/Q) ratio, contributing to overall improvements in pulmonary function [11]. In this case, the improvement achieved with conventional respiratory rehabilitation alone was minimal. Considering the patient's initial general medical condition, we can assume that the prolonged period of bedside treatment, due to the patient's difficulty in maintaining a sitting position, contributed to the limited progress. As the patient’s general condition improved, conventional respiratory rehabilitation could be performed more actively in combination with aerobic exercise and activities such as wheelchair transfer training. This integrated approach may have produced a synergistic effect, contributing to improvements in ventilation-perfusion (V/Q) matching and an overall increase in respiratory effort.
Previous studies have reported that patients with SCI commonly exhibit a restrictive lung pattern when assessed using spirometry [12]. However, in this case, the patient initially presented with an obstructive lung pattern. While no pulmonary abnormalities were observed on the initial chest CT taken at the time of injury, follow-up chest CT and X-ray after spinal fusion surgery revealed atelectasis in the right upper lobe and both lower lobes. Despite undergoing pulmonary rehabilitation, persistent atelectasis in both lower lobes was observed. However, after initiating aerobic exercise, only a small amount of atelectasis remained in the right lower lobe. These findings suggest that the obstructive lung pattern observed in this patient was likely attributable to atelectasis.
The patient’s body weight was not regularly monitored during the inpatient rehabilitation period, and thus the extent of weight loss or gain and its possible impact on pulmonary function throughout the recovery could not be determined. This is recognized as a limitation of the current case.
In spinal cord injury patients undergoing tracheostomy, moderate to high-intensity aerobic exercise may be attempted to facilitate decannulation. Further large-scale controlled studies and investigation into the effects of low-intensity aerobic exercise on PCF, FVC, and FEV1 are warranted.
